
MYOMECTOMY
Frequently Asked Questions
Yes, for emergency services
Menstrual pain, infertility, vaginal infection, irregular periods,uterine fibroids & hysteroscopy.
Adolescent Menstrual Problems,Menopause clinic, Female genital cancer screeing.
Fibroid Uterus, Polyps, Dysfunctional Uterine Bleeding, Genital cancers.
Pelvic examination, Ultrasonography, Hysteroscopy, D&C Biopsy, Colposcopy & Cervical Biopsy, MRI, Laboratory Investigation
Removal of Uterus
Laparoscopic Total
Hysterectomy (TLH),
Total abdominal hysterectomy (TAH),
Non Descent Vaginal
Hysterectomy (NDVH),
Vaginal Hysterectomy (VH).
Hysterectomy (TLH),
Total abdominal hysterectomy (TAH),
Non Descent Vaginal
Hysterectomy (NDVH),
Vaginal Hysterectomy (VH).
Lifestyle has a considerable influence on periods. Poor diet and taking a lot of stress can delay periods by several days or even a month. Other reasons may include polycystic ovarian syndrome for which Gynecologists may prescribe birth control pills.
Vaginal discharge is the body’s cleansing mechanism. It is normal to have clear or milky discharge, but in case you notice a variation in the color, odor or volume (unusually high), it may be a sign of infection. Rush to your doctor for immediate evaluation.
Urinary tract infection can quickly spread inside your system and causes a burning sensation while urinating. It might as well be a temporary infection, but the sure-shot way to know is to ask an expert and get yourself examined.
Risks
- Myomectomy has a low complication rate. Still, the procedure poses a unique set of challenges.
- Risks of myomectomy include
- Excessive blood loss
- Scar Tissue
- Pregnancy or Childbirth complications
- Rare chance of hysterectomy
- Rare chance of spreading a cancerous tumor
Strategies to prevent possible surgical complications
To minimize risks of myomectomy surgery, your doctor may recommend:
Iron supplements and vitamins
If you have iron deficiency anemia from heavy menstrual periods, your doctor might recommend iron supplements and vitamins to allow you to build up your blood count before surgery.


Hormonal treatment
Treatment with hormones prior to surgery is another method for treating anaemia. To stop or lessen your menstrual flow, your doctor can recommend a gonadotropin-releasing hormone (GnRH) agonist, birth control tablets, or another hormonal drug.
Some hormonal treatments, like GnRH agonist therapy, can also shrink your fibroids and uterus to the point where your surgeon can perform surgery with minimally invasive techniques, like laparoscopic surgery rather than open surgery or a smaller, horizontal incision.
Preparation for the surgery
Food and medications
Prior to your procedure, you must fast—that is, refrain from eating or drinking anything. Observe the advice of your doctor on the precise number of hours.
In the days leading up to surgery, if you take medication, discuss with your doctor whether you should change your regular drug schedule. If you take any over-the-counter drugs, vitamins, or other dietary supplements, let your doctor know.
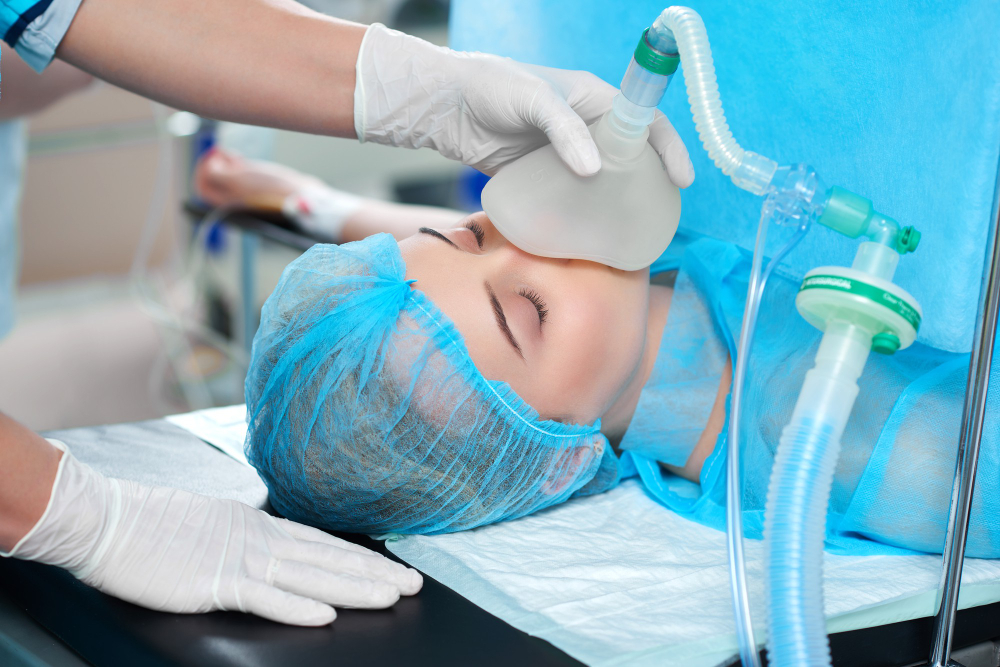
Anaesthesia
You can experience one of the following anaesthesia kinds depending on your procedure:
General anesthesia
With general anaesthesia, a tube will be put in your throat while you are completely unconscious. Laparoscopic myomectomy, abdominal myomectomy, and occasionally hysteroscopic myomectomy all involve the use of general anaesthesia.
Monitored anesthesia care
You normally don’t recall anything and feel completely unconscious when under this sort of anaesthesia. No tube has been inserted into your throat. Hysteroscopic myomectomy is frequently performed with MAC because it’s a less intrusive operation and necessitates less anaesthesia.
Depending on the size, number and location of your fibroids, your surgeon may choose one of three surgical approaches to myomectomy.
Spinal Anaesthesia
Combined Spinal Epidural Anaesthesia
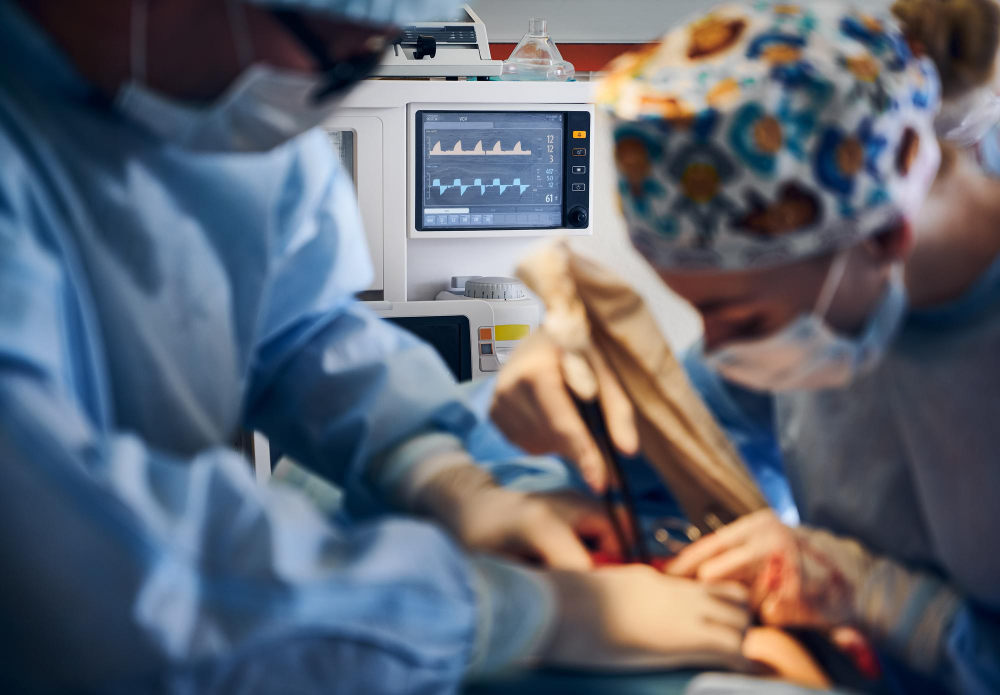
Abdominal myomectomy
In abdominal myomectomy (laparotomy), your surgeon makes an open abdominal incision to access your uterus and remove fibroids. Your surgeon will generally prefer to make a low, horizontal (“bikini line”) incision, if possible. Vertical incisions are needed for larger uteruses.
Laparoscopic
In laparoscopic or robotic myomectomy, both minimally invasive procedures, your surgeon accesses and removes fibroids through several small abdominal incisions.

robotic myomectomy
Compared with women who have a laparotomy, women who undergo laparoscopy have less blood loss, shorter hospital stays and recovery, and lower rates of complications and adhesion formation after surgery. There are limited comparisons between laparoscopic and robotic myomectomy. Robotic surgery may take longer and be more costly, but otherwise few differences in outcomes are reported.
Laparoscopic myomectomy
Your surgeon makes a small incision in or near your bellybutton. Then he or she inserts a laparoscope — a narrow tube fitted with a camera — into your abdomen. Your surgeon performs the surgery with instruments inserted through other small incisions in your abdominal wall.

Robotic myomectomy
Your surgeon inserts instruments through small incisions similar to those in a laparoscopic myomectomy, and then controls movement of the instruments from a separate console. Some surgeons are now performing single-port (one incision) laparoscopic and robotic myomectomies.
Sometimes, the fibroid is cut into pieces (morcellation) and removed through a small incision in the abdominal wall. Other times the fibroid is removed through a bigger incision in your abdomen so that it can be removed without being cut into pieces. The fibroid may also be removed through an incision in your vagina (colpotomy).
Hysteroscopic myomectomy
To treat smaller fibroids that bulge significantly into your uterus (submucosal fibroids), your surgeon may suggest a hysteroscopic myomectomy. Your surgeon accesses and removes the fibroids using instruments inserted through your vagina and cervix into your uterus.

Outcomes from myomectomy may include
Symptom relief. After myomectomy surgery, most women experience relief of bothersome signs and symptoms, such as excessive menstrual bleeding and pelvic pain and pressure.
Fertility improvement. Women who undergo laparoscopic myomectomy, with or without robotic assistance, have good pregnancy outcomes within about a year of surgery. After a myomectomy, suggested waiting time is three to six months before attempting conception to allow your uterus time to heal
+91 8660534318
South Mark Gynaecology Clinic
3rd Main Rd, opposite Star Market, near ISRO layout, Banashankari 5th Stage, ISRO Layout, Bengaluru, Karnataka 560078
Zymus Hospital
No.1, K NO. 92, Nanjappa Complex, Kanakapura Rd, Raghuvanahalli, Bangalore City Municipal Corporation Layout, Bengaluru, Karnataka 560062
© 2024. All Rights Reserved.

